Can hanging out with tall people during development make you taller? One potential mechanism for how your communities genes may affect yours may be via biophotons.
The impact of physical connectedness on body height in Swiss conscripts.
“Human populations differ in height. Recent evidence suggests that social networks{who you hang out with} play an important role in the regulation of adolescent growth and adult height. We further investigated the effect of physical connectedness on height.
We considered Switzerland as a geographic network with 169 nodes (district capitals) and 335 edges (connecting roads) and studied effects of connectedness on height in Swiss conscript from 1884 – 1891, 1908 – 1910, and 2004 – 2009. We also created exponential-family random graph models to separate possible unspecific effects of geographic vicinity.
In 1884 – 1891, in 1908 – 1910, and in 2004 – 2009, 1(st), 2(nd) and 3(rd) order neighboring districts significantly correlate in height (p < 0.01). The correlations depend on the order of connectedness, they decline with increasing distance. Short stature districts tend to have short, tall stature districts tend to have tall neighbors. Random network analyses suggest direct road effects on height. Whereas in 1884 – 1891, direct road effects were only visible between 1(st) order neighbors, direct road effects extended to 2(nd) and 3(rd) in 1908 – 1910, and in 2004 – 2009, also to 4(th) order neighbors, and might reflect historic improvements in transportation. The spatial correlations did not significantly change when height was controlled for goiter (1884 – 1889) and for median per capita income (2006), suggesting direct road effects also in goiter-allowed-for height and income-allowed-for height.
Height in a district depends on height of physically connected neighboring districts. The association decreases with increasing distance in the net. The present data suggest that people can be short because their neighbors are short; or tall because their neighbors are tall (community effect on growth). Psycho-biological effects seem to control growth and development within communities that go far beyond our current understanding of growth regulation.”
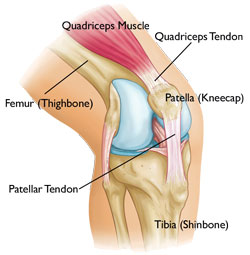
Final height, target height and the community.
“Height varies with age, and it varies with historic time. Final height is determined by endocrine parameters and genetics, by nutrition and health, by environmental factors, by birth weight, early growth, BMI, and developmental tempo. European populations of the 19th century were short, but their shortness did not result from growth impairment at all ages. In those days, shortness was mainly due to a significantly blunted adolescent growth spurt. New modelling approaches suggest an independent regulation of adolescent growth and final height: the target for growth and final height appears to be set by the community{hanging around with probasketball players may make you taller?}. In order to test this hypothesis, we formed a geographic network of Switzerland consisting of 169 nodes (district capitals) and 335 connecting edges (roads), and investigated military conscript data obtained between 2004 and 2009. Average height of Swiss military conscripts was 178.2 cm (SD 6.5 cm). But conscripts from first order neighbouring districts were more similar in height than expected. Short stature districts have short, tall stature districts have tall neighbours. We found significant height correlations between 1st (r=0.58), 2nd (r=0.64), 3rd (r=0.45) and even 4th order neighbours (r=0.42). It appears that tall stature communities generate tall people, short stature communities generate short people, and migrants orientate towards the new height target of their host population (community effect on growth){So independent of genes from the community newborn migrants will be taller or shorter based on the community}. ”
Modeling determinants of growth: evidence for a community-based target in height?
“community-based target seeking in growth”
“adolescent height converges toward the average of the population. Height tends to cluster. The within-population variation of height is narrow.”
“Height differences are small throughout childhood but markedly increase during adolescence.”
“the smaller the adolescent is compared with past mean average height, the more the adolescent grows during puberty.”<-So according to this theory, if you are going through puberty and hang out with pro-basketball players you will grow taller than expected and at a faster rate.
“Short stature in cystic fibrosis results from tempo deceleration. Cystic fibrosis patients grow poorly at all ages (they have suboptimal peak height velocity and late pubertal growth, influenced by disease severity) but eventually achieve normal final height. ”
” tall communities generate tall people even in the presence of unfortunate living conditions”
According to Dose-dependent effect of growth hormone on final height in children with short stature without growth hormone deficiency.,exogenous administration of GH increased height by about 1 inch. The authors of this study suggest that living around taller people could increase GH production as depression decreases GH production establishing a link between mental state and GH production.
Here’s a study that suggests that IGF-1 levels may play a role in the community effect on height. Although it does not seem to be a strictly linear relationship between IGF-1 levels and height. Height is more complex than that.
Sex, Sport, IGF-1 and the Community Effect in Height Hypothesis.
“We test the hypothesis that differences in social status between groups of people within a population may induce variation in insulin-like growth factor-1(IGF-1) levels and, by extension, growth in height{so “positive thinking” increases height via IGF-1 but again the relationship is more complex than IGF-1 increases height}. This is called the community effect in height hypothesis. The relationship between IGF-1, assessed via finger-prick dried blood spot, and elite level sport competition outcomes were analysed for a sample of 116 undergraduate men and women. There was a statistically significant difference between winners and losers of a competition. Winners, as a group, had higher average pre-game and post-game IGF-1 levels than losers. We proposed this type of difference as a proxy for social dominance. We found no evidence that winners increased in IGF-1 levels over losers or that members of the same team were more similar in IGF-1 levels than they were to players from other teams. These findings provide limited support toward the community effect in height hypothesis. The findings are discussed in relation to the action of the growth hormone/IGF-1 axis as a transducer of multiple bio-social influences into a coherent signal which allows the growing human to adjust and adapt to local ecological conditions.”
So it seems that the relationship as described here is that winners are more likely to have higher IGF-1 levels rather than winning increasing IGF-1 levels.
“Children and adolescents with pituitary gigantism have an excessive production of GH, and IGF-1 levels are elevated.”<-But again it seems as though there’s more to gigantism than excessive GH.
“the positive association between variation in IGF-1 levels and height, across the range from deficiency to excess, helps to explain differences in stature within and between human populations.”
” there is evidence for a new parameter that they define as ‘past relative height.’ This parameter operates during the adolescent growth period to adjust the growth rate of an individual toward the average height of her/his immediate community.”
“… the smaller the adolescent is compared with past mean average height [of the community], the more the adolescent grows during puberty”
Surprisingly the scientists found that women in sports tended to have higher IGF-1 levels than men in sports.
“Women, but not men, showed a significant association between their father’s social class and their own adult IGF-1 levels.”